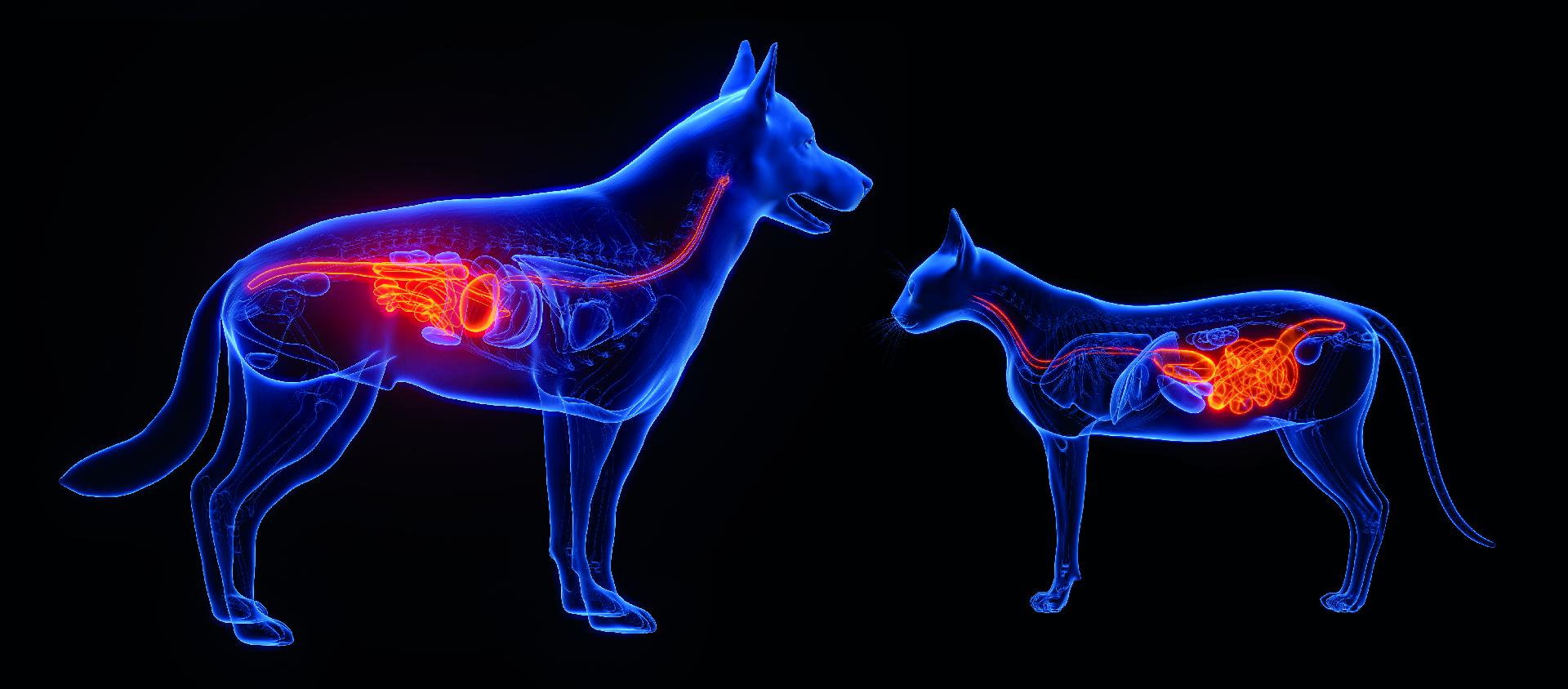
The intestinal epithelium acts as a physical and immune barrier, preventing the content present in the intestinal lumen from diffusing to other tissues and organs and compromising their homeostasis. Adverse food reactions are abnormal responses to an ingested food and can be divided into 2 main groups:
1) Food intolerance or intoxication, reaction without the involvement of the immune system;
2) Food hypersensitivity or allergy, immune-based food reaction;
When the adverse reaction does not involve the immune system, the terms intolerance and food poisoning can be used, related to metabolic, idiosyncratic, pharmacological reactions and ingestion of toxins present in some food.
Food poisoning results from the direct action of a food or food additive. Examples include excessive nutrient intake (vitamin A or D intoxication, selenium), food contaminated with microorganisms or their toxic metabolites (decaying material, mycotoxins), specific foods (onions, chocolates), or food preservatives (benzoic acid or propylene glycol in cats).
Gluten-induced enteropathy (celiac disease) is a major food intolerance, which causes chronic inflammation of the small intestine. "Gluten" is a crude mixture of gliadin and glutenin, and is normally well digested by pancreatic enzymes in the intestinal lumen, and intracellular enzymes in the brush border of the mucosa. Familial gluten-sensitive enteropathy has been described in Irish setters. However, this sensitivity can affect a larger number of breeds of dogs and cats. In this breed, this pathology can be observed between four and seven months of age as an inability to gain weight accompanied by chronic diarrhea (Garden et al., 2000).
Food hypersensitivity or, more simply, food allergy, is included in the differential diagnosis of dogs and cats affected by clinical manifestations associated with skin diseases. It represents an immune-based adverse reaction to food as well as food anaphylaxis.
Despite the relatively low prevalence of food hypersensitivity in small animals (compared to other allergies such as atopic dermatitis and flea allergy dermatitis), many animals have a multifactorial etiology, which means they are allergic to flea saliva, flea food, and dust mites at the same time. Thus, in supposedly allergic animals, it is essential to determine whether or not the food participates in the clinical picture.
Food allergies usually occur as non-seasonal itchy dermatitis, with or without gastrointestinal signs. Pruritus varies in severity, and the distribution of the lesion is often indistinguishable from that seen in atopic dermatitis triggered by environmental allergens. The feet, face, armpits, perineal region, groin region, and ears are often affected. It should always be suspected in dogs with pruritic otitis (external unilateral or bilateral), accompanied by secondary bacterial or fungal infections.
Generally, the main food allergens are water-soluble glycoproteins, which have a molecular weight ranging from 10 to 70 kD (thousand daltons) and are stable to heat, acid, and protease treatment. Meat, dairy, and wheat are the ingredients that most commonly cause adverse food reactions in dogs. Specific food allergens identified in dogs include chicken serum albumin, bovine IgG (milk and beef), sheep IgG (lamb), muscle phosphoglucomutase (beef, lamb), and Gly 50 and 75 kD soy proteins. Meat, soy, rice, dairy products, and fish are the ingredients that most commonly cause adverse food reactions in cats.
Elimination challenge tests confirm the diagnosis of an adverse reaction to a specific food. Resolution of clinical signs occurs after food elimination is present in the patient's diet, followed by a signal return when the patient faces the original food.
How to adjust the diet for adverse reactions to food?
Theoretically, the treatment would eliminate the agent causing the adverse reaction from the animal's diet. This option is more feasible when we talk about adverse reactions that do not involve the immune system since it is easy to identify which ingredient or food is causing the direct reaction of intolerance or intoxication to the organism.
Food allergy is an immune reaction to proteins ingested in the diet that are mistakenly identified by the body as antigens, generating an immune response that involves GALT (gut-associated lymphoid tissue).
As protein is an essential macronutrient for dogs and cats and we cannot eliminate it from their diets, our strategy in pet food is to include protein sources in quantity and quality, which will be key factors in the management of adverse food reactions in dogs and cats.
Thus, the protein/energy ratio in hypoallergenic diets is a parameter of great importance for the formulation since the denser the diet, the less protein the animal will ingest. It would be interesting if the hypoallergenic rations had ME equal to or greater than 4000 Kcal/kg, both for cats and dogs.
However, not only the % of crude protein inclusion in hypoallergenic diets should be considered; the type of protein is a key factor to improve the immune response. Using unprecedented protein sources or synthetic amino acids is an excellent strategy since the animal has never had contact with them, and their immune system does not identify them. Some products replace beef or chicken with exotic meats for pets, such as lamb, salmon, rabbit, venison, ostrich, among others. However, the cost and availability of these proteins make it difficult to produce and market this type of food.
The immune system recognizes proteins with a molecular weight greater than 5 kD; those with a lower weight are absorbed and are not identified. Currently, the most commercialized hypoallergenic foods are those formulated with hydrolyzed protein. They undergo a denaturation and fragmentation process by chemical reactions.
New products with the analgesic concept are coming onto the market; in addition to hydrolyzing the protein sources, the other ingredients are, for example, protein-free; only the starch fraction of the carbohydrate sources are used to ensure that no protein is produced. They do not even have plant-based allergens.
The ratio between ω6 and ω3 fatty acids in animal tissues can be modulated through diet and thus influence the inflammatory response of animal skin. To improve the performance of polyunsaturated fatty acids, there must be an optimal ratio between them. According to Reinhart et al. (1996), a ω6:ω3 ratio between 5:1 and 10:1 can significantly reduce itching conditions. Vaughn et al. (1994) determined an optimal ω6:ω3 ratio of 10:1 to 5:1 for adult dogs, while Wander et al. (1997) studying elderly dogs, found a significant decrease in prostaglandin E2 (PGE2) only with the ω6:ω3 ratio of 1.4:1.
By: Gabriela S.C.P. Corte Real, Ludmila Barbi, Erika Stasieniuk
Source: All Pet Food
You could be interested: Common black fly larvae added to list of alternative protein source in animal feed
About author
Erika StasieniukErika Stasieniuk is a Zootechnician and Doctor in Nutrition and Feeding of Dogs and Cats at UFMG. She is a founding partner of SFA Consultoria, whose objective is to help food and ingredient companies for dogs and cats develop their products and produce safe and quality food.